Breast Cancer Treatment Options
Because there are several types of breast cancer, there are also several types of breast cancer treatment. At Cancer Care Centers of Brevard, our dedicated team of medical oncologists use the latest breast cancer treatment technologies to create a unique treatment plan for each patient. They are available to take questions and guide you through the process of starting a cancer treatment plan that is right for you.
The following is a broad description of breast cancer treatments that may be used as part of your treatment plan. This may include one or a combination of the following treatments including:
- Breast Cancer Surgery
- Radiation Therapy
- Chemotherapy
- Hormone Therapy
- Targeted Therapy
- Immunotherapy
- Clinical Trials
Breast Cancer Surgery
Most women will receive surgery as part of their breast cancer treatment. Your oncologist and breast surgeon will discuss your options to compare the benefits and risks of each, and describe how each will change the way you look:
Breast-Sparing Surgery
Also called breast-conserving surgery, this operation removes the cancer rather than the breast. It can be done as a lumpectomy or segmental mastectomy (also called a partial mastectomy). Sometimes an excisional biopsy is the only surgery a woman needs because the surgeon was able to remove the whole lump.
Breast-conserving surgery involves removing the cancer in the breast and some tissue around it. The surgeon may also remove lymph nodes under the arm, and sometimes removes part of the lining over the chest muscles under the tumor.
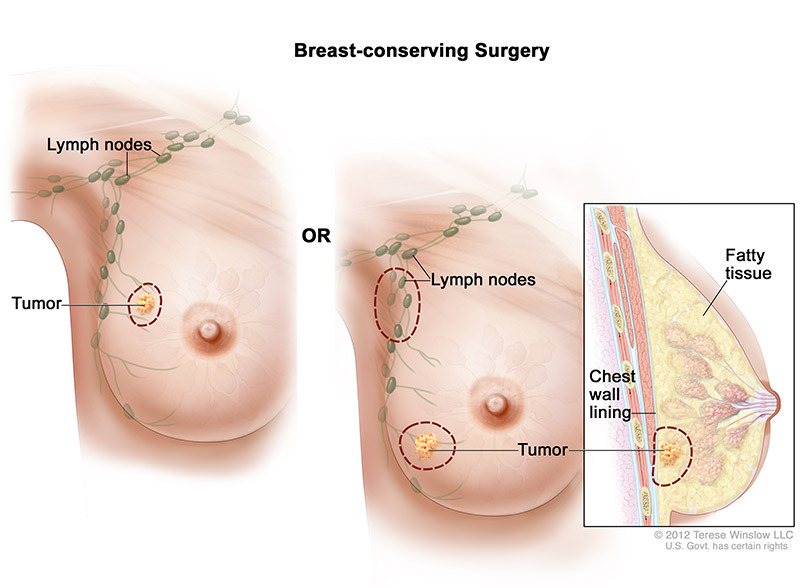
Mastectomy
This operation removes the entire breast (or as much of the breast tissue as possible) and possibly some of the lymph nodes. This is called a total mastectomy. Another option is a modified radical mastectomy, where the entire breast and most or all of the lymph nodes are removed. In some cases, a skin-sparing mastectomy may be an option. For this approach, your surgeon removes as little skin as possible.
Total (simple) mastectomy involves the surgeon removing the whole breast. Some lymph nodes under the arm may also be removed.
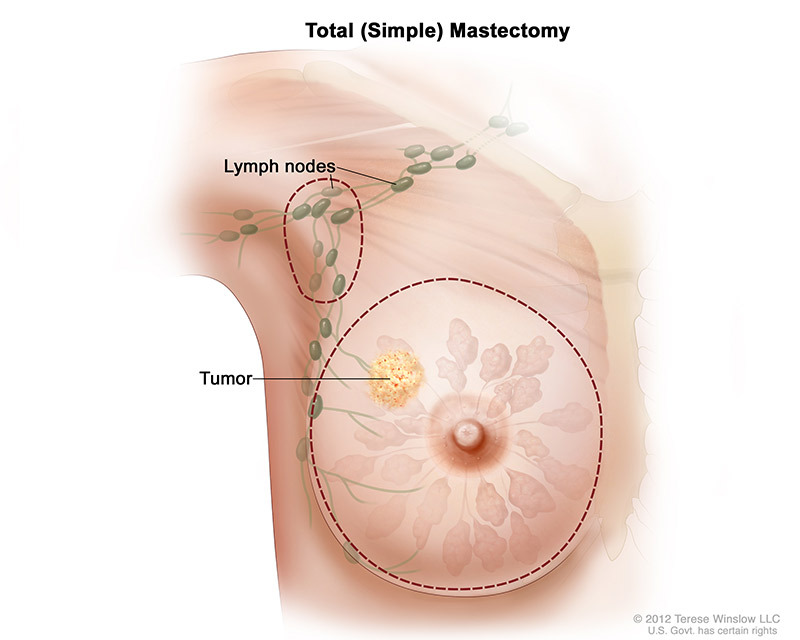
Modified radical mastectomy involves the surgeon removing the whole breast, and most or all of the lymph nodes under the arm. In many cases, the lining over the chest muscles is also removed. A small chest muscle may be taken out to access and remove the lymph nodes easier.
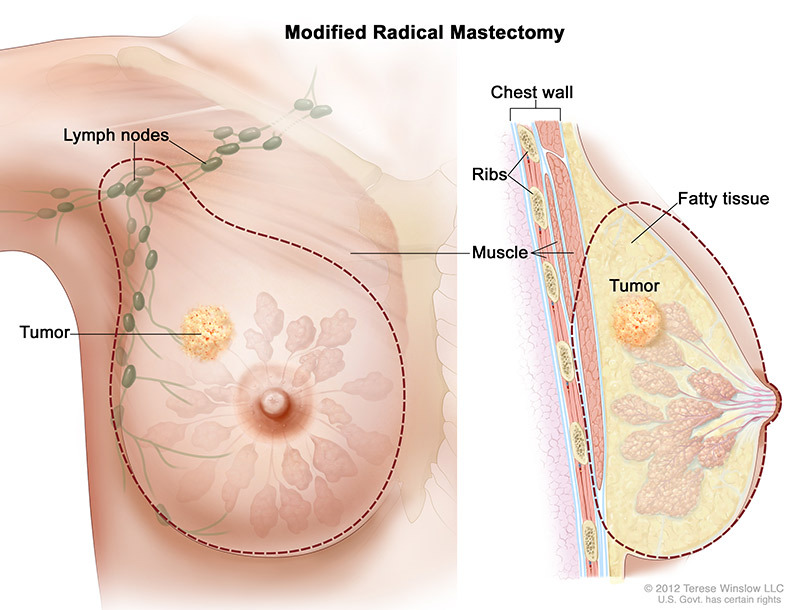
The surgeon usually does a sentinel lymph node biopsy at this time to see if there may be lymph node involvement.
You may choose to have breast reconstruction, which involves using plastic surgery to rebuild the shape of the breast. It may be done at the same time as the cancer surgery or later. If you’re considering breast reconstruction, you may wish to talk with a plastic surgeon before having cancer surgery.
Radiation Therapy for Breast Cancer
To destroy breast cancer cells that remain in the area after surgery, radiation therapy may be recommended. It could also be given to the nearby lymph nodes. For women who had a modified radical mastectomy, it may or may not be recommended depending on the size of the tumor, whether it has spread to lymph nodes and how many lymph nodes.
Our breast cancer treatment team will review your specific situation to determine what is most likely to work best with the least side effects.
- External Radiation Therapy comes from a large machine outside the body. Treatments will be given at a hospital or clinic for treatment and last five days a week for four to six weeks. External radiation is the most common type used for breast cancer.
The radiation oncologists at Cancer Care Centers of Brevard also offer a more advanced approach called hypofractionated radiation therapy that gives the same dose of radiation in a shorter time period. Instead of a 6-8 week course of radiation therapy, the same results can be achieved in 4-5 weeks by giving a higher dose of radiation at each treatment.
The specific number of treatment sessions depends on where the cancer is located, size, and the patient’s overall health condition. The shorter course of radiation treatments is made possible through more advanced delivery methods. By using the technology to precisely aim the rays of radiation, the cancerous cells are treated with a higher dose while sparing nearby organs and tissues. - High Dose Rate (HDR) Breast Brachytherapy can be used to treat early-stage breast cancer. The oncologist places one or more thin tubes inside the breast through a tiny incision. Most commonly, radioactive pellets are loaded into the tubes each day for about 5 days and pointed at the area where there was cancer. At the end of the treatment, the device with the tubes is removed. This may be done instead of surgery for some patients or it is used after breast-conserving surgery to ensure that all the cancer cells in the surgical area are destroyed.
RELATED READ:
What You Should Know About Radiation Therapy for Breast Cancer Treatment
Breast Cancer Chemotherapy
Chemotherapy drugs kill cancer. They are usually given through a vein (intravenous) or as a pill. If chemotherapy is part of your treatment plan, you will probably receive a combination of drugs based on the type, stage and grade of breast cancer you have.
Chemotherapy for breast cancer treatment is given in cycles. Typically, this can be once a week or every few weeks, over the course of several months.
Some anticancer drugs cause damage to the ovaries. If you have not gone through menopause yet, you may experience symptoms such as hot flashes and vaginal dryness. Your menstrual periods may no longer be regular or may stop. You may become infertile (unable to become pregnant). For women over the age of 35, this damage to the ovaries is likely to be permanent. Breast cancer chemotherapy often causes hair loss. Talk to the cancer care team to talk about options for reducing hair loss and preparing for what you may experience.
Hormone Therapy to Treat Breast Cancer
If lab tests show that the tumor in your breast has hormone receptors, then hormone therapy may be an option. Hormone therapy, also sometimes called anti-hormone treatment, keeps cancer cells from getting or using the natural hormones (estrogen and progesterone) they need to grow.
Hormone therapy is usually given along with other therapies (adjuvant) and may be recommended for several years after your other breast cancer treatments are complete.
Hormone Therapy Options Before Menopause
If you have not gone through menopause, the options include:
- Tamoxifen: This drug can prevent the original breast cancer from returning and also helps prevent the development of new cancers in the other breast. As treatment for metastatic breast cancer, tamoxifen slows or stops the growth of cancer cells that are in the body. Tamoxifen comes in pill form and is taken every day for five years. Generally, the side effects of tamoxifen are similar to some of the symptoms of menopause with the most common being hot flashes and vaginal discharge. Others are irregular menstrual periods, thinning bones, headaches, fatigue, nausea, vomiting, vaginal dryness or itching, irritation of the skin around the vagina, and skin rash. Serious side effects are rare, but they include blood clots, strokes, uterine cancer, and cataracts. You may want to read the NCI fact sheet Tamoxifen.
- LH-RH agonist: This type of drug can prevent the ovaries from making estrogen, which causes the estrogen level to fall slowly. This type of drug may be given by injection under the skin in the stomach area. Side effects include hot flashes, headaches, weight gain, thinning bones, and bone pain. Leuprolide and goserelin are examples of LH-RH agonists.
- Surgery to remove your ovaries: Your ovaries are your body’s main source of estrogen until you go through menopause. When the surgeon removes your ovaries, this source of estrogen is also removed. (A woman who has gone through menopause wouldn’t benefit from this kind of surgery because her ovaries produce much less estrogen.) When the ovaries are removed, menopause occurs right away. The side effects are often more severe than those caused by natural menopause. Your healthcare team can suggest ways to cope with these side effects.
Hormone Therapy for Hormone-Receptor-Positive Breast Cancer
If your breast cancer was hormone-receptor-positive you may be a candidate for hormone therapy drugs that will help your body from producing too much of the hormone that fueled the breast cancer. These are taken every day for 5-10 years after diagnosis.
Common hormone therapies for breast cancer include:
- Tamoxifen: Premenopausal and post-menopausal women are able to receive tamoxifen for 2-5 years after a breast cancer diagnosis. If tamoxifen is given for less than five years, then an aromatase inhibitor often is given to supplement the remaining years for postmenopausal women. Hot flashes, night sweats, and vaginal dryness are common side effects as well as an increased risk of blood clots and stroke.
- Aromatase inhibitors: This type of drug prevents the body from making a form of estrogen (estradiol). This hormone therapy is for post-menopausal women. Common side effects include hot flashes, nausea, vomiting, and painful bones or joints. Serious side effects include thinning bones and an increase in cholesterol. Anastrozole, exemestane, and letrozole are examples of aromatase inhibitors.
Targeted Therapy
Another breast cancer treatment approach is targeted therapy. Targeted therapy uses drugs that block the growth of breast cancer cells. For example, targeted therapy may block the action of the HER2 protein that stimulates the growth of breast cancer cells.
Trastuzumab (Herceptin®), lapatinib (TYKERB®), or other approved targeted therapies for breast cancer may be given to a woman whose lab tests show that her breast tumor has too much HER2.
RELATED READ:
HER2-Low Breast Cancer Treatment Breakthrough for Inoperable or Metastatic Breast Cancer

Immunotherapy for Breast Cancer
Breast cancer cells can hide as healthy cells so the checkpoints don't detect them to attack the cancer. Research has found a way to make your body's immune systems fight cancer cells by using immunotherapy drugs.
A few immunotherapies have been FDA-approved for breast cancer treatment. These immune checkpoint inhibitors make it possible for the body to recognize the difference between cancer cells and healthy cells. Identifying the cancer cells helps the immune system do its job and attack the unhealthy cells.
Patients with triple-negative breast cancer have found immunotherapy effective when combined with chemotherapy. Learn more about triple-negative breast cancer treatments in our blog.
Clinical Trials for Breast Cancer Treatment
Cancer Care Centers of Brevard offers access to the latest cancer research clinical trials in Brevard County, Florida. Our participation in breast cancer research allows us to provide new treatment options to patients who may not respond to the standard breast cancer treatment protocols. Treatments being researched by our breast cancer specialists have already been proven safe for humans. However, every patient who volunteers to participate in a breast cancer trial is carefully monitored to determine the treatment's effectiveness. Contact our breast cancer doctors at our cancer centers where clinical trials for breast cancer are available.
The Latest Breast Cancer Treatments Available in Brevard County
If you or a loved one have been recently diagnosed with breast cancer, Cancer Care Centers of Brevard is here to help you through your journey. Our breast cancer specialists offer the latest treatments available with personalized treatment plans tailored to you. Our cancer centers are located throughout Brevard County, including Palm Bay, Rockledge, Melbourne, and Merritt Island, FL.